TL;DR:
- The UK offers NHS, private, and online therapy options, each with different costs and wait times.
- Preparing detailed personal information and understanding confidentiality are key before starting support.
- Progress in therapy is gradual; small steps and tracking help maintain motivation and assess effectiveness.
Your step-by-step guide to mental health support in the UK
Seeking help for anxiety or depression can feel overwhelming, especially when you are unsure where to begin, what things cost, or whether your privacy will be protected. The sheer number of options, from NHS services to private online platforms, makes it easy to feel paralysed before you have even taken a single step. Many adults in the UK quietly struggle for months, or even years, before accessing any form of support. This guide cuts through the uncertainty. It provides clear, practical steps to help you identify the right path, prepare effectively, and begin receiving the confidential, affordable mental health support you need.
Table of Contents
- Understanding your options for mental health support
- What you need to prepare before seeking help
- Step-by-step guide to starting mental health support
- What to expect and how to monitor your progress
- Why most people give up and how you can break the cycle
- Take your next step to confidential support
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Know your options | NHS, private, and online therapy each have strengths—compare them for your needs. |
| Prepare smartly | List your needs and priorities before you start searching or booking therapy. |
| Take small steps | The key is acting on one step at a time, not finding a perfect solution from the start. |
| Check your progress | Regularly review how you feel and adjust your approach for better results. |
Understanding your options for mental health support
The UK offers a wider range of mental health support options than most people realise. Understanding what is available helps you make an informed decision rather than a default one.
The three main routes
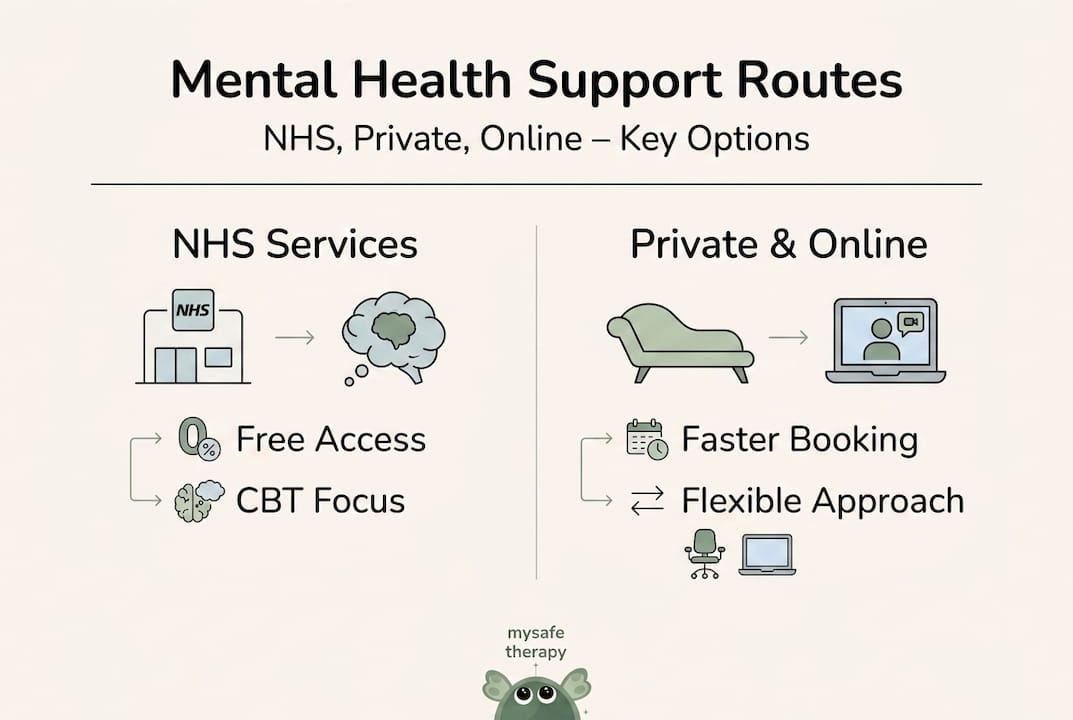
The three primary routes to mental health support in the UK are NHS services, private therapy, and online therapy platforms. Each has distinct characteristics across cost, speed, flexibility, and confidentiality.
| Route | Cost | Wait time | Flexibility | Confidentiality |
|---|---|---|---|---|
| NHS Talking Therapies | Free | 4 to 18 weeks | Limited | High |
| Private therapist | £50 to £120 per session | Days to 1 week | High | High |
| Online therapy platform | £30 to £70 per session | 24 to 72 hours | Very high | High |
The NHS provides free access to structured, evidence-based therapies, primarily Cognitive Behavioural Therapy (CBT). CBT is a structured talking therapy that helps you identify and change unhelpful thought patterns. The IAPT programme treats over one million people annually and research shows CBT performs comparably to medication for mild to moderate anxiety and depression. However, NHS waiting lists can be long, sometimes running to several months, which may not suit everyone.

Private therapy offers faster access and greater choice of therapist. You can often find an appointment within days. The trade-off is cost, which is a genuine barrier for many people. Online therapy platforms offer a middle ground. They tend to be more affordable than traditional private therapy, often available within 24 to 48 hours, and accessible from home, which removes travel as a barrier. Platforms like MySafeTherapy offer formats including video, chat, and avatar-based sessions, giving you genuine flexibility.
When a hybrid approach makes sense
Some people find that a hybrid approach works best. This means self-referring to NHS Talking Therapies while simultaneously using an online platform for immediate support. It is a practical way to ensure you are not left without help during a long wait. Personalised therapy that matches your schedule, budget, and preferred format is more likely to be effective than a one-size approach.
Here are some factors to weigh when choosing:
- Cost: Can you afford private therapy, or do you need a free or lower-cost option?
- Speed: How urgently do you need support?
- Format: Do you prefer face-to-face video, written chat, or anonymous avatar-based sessions?
- Schedule: Do you need evening or weekend availability?
- Privacy: Do you want sessions that are completely separate from your GP record?
Pro Tip: If cost is a barrier but NHS waits feel too long, look for online platforms that offer sliding-scale pricing or introductory sessions. Many BACP-registered therapists work across both NHS and private settings.
What you need to prepare before seeking help
With an overview of your options, the next step is to get prepared so you can make the most out of any support path you pursue. Preparation saves time, reduces anxiety during sign-up, and helps you communicate clearly with a therapist from the start.
Key information to gather
Before contacting any service, it is helpful to gather the following:
- Your symptoms: Note when they started, how frequent they are, and how they affect daily life. Be specific. "I feel anxious most mornings and struggle to leave the house three days a week" is far more useful than "I feel low."
- Medical history: Include any existing diagnoses, medications, or previous mental health treatment. Services will ask about this during assessment.
- What you want from therapy: Think about your goals. Do you want to manage panic attacks, improve your sleep, reduce low mood, or address relationship difficulties?
- Practical needs: Consider your availability, preferred session format, and any specific requirements such as a therapist of a particular gender or cultural background.
When you contact a service, whether NHS or private, you will typically be asked a short set of questions to assess your needs. These often include standardised questionnaires such as the PHQ-9 for depression and GAD-7 for anxiety. These are simple scoring tools that help services triage and match you appropriately. Understanding this process in advance reduces any surprise or discomfort.
Checking confidentiality arrangements
Confidentiality is a major concern for many people, and rightly so. Private and online therapy services generally do not share information with your GP without your consent, unless there is a serious risk of harm. NHS Talking Therapies operate within NHS data systems, so records may be accessible to your GP. If privacy from your GP is a priority, online therapy platforms may be the better fit. Always check the platform's privacy policy and ask directly before you begin.
Research consistently shows the consequences of long NHS waits. As noted in comparisons of private vs NHS care, the NHS is free but extended waiting periods can lead to symptom deterioration, whereas private and online options offer speed and flexibility at a financial cost. A hybrid approach is often recommended for those who need timely mental health management tips while waiting for longer-term NHS support.
The table below summarises what to expect during sign-up for different service types:
| Service type | Sign-up process | Assessment type | Time to first session |
|---|---|---|---|
| NHS Talking Therapies | Online self-referral or GP | PHQ-9, GAD-7 questionnaires | 4 to 18 weeks |
| Private therapist | Phone or email enquiry | Initial consultation call | 1 to 7 days |
| Online therapy platform | Digital form, account creation | In-app questionnaire | 24 to 72 hours |
Pro Tip: Before you sign up anywhere, list your top three priorities, for example, cost, speed, and therapist gender. Matching those three criteria will quickly narrow your options and reduce decision fatigue.
Familiarising yourself with common therapy techniques beforehand can also help you feel less apprehensive about your first session.
Step-by-step guide to starting mental health support
Once you have your preparation sorted, use this step-by-step approach to get the support you need. This section covers both the NHS and private or online routes so you can follow whichever applies to you.
Accessing NHS Talking Therapies
- Visit the NHS Talking Therapies website: Go to nhs.uk and search for "Talking Therapies" or "IAPT" to find your local service. Every area of England has one.
- Complete the self-referral form: Most services accept online self-referrals without a GP appointment. The form asks about your symptoms, contact details, and any previous treatment. It takes around ten to fifteen minutes.
- Attend your assessment appointment: A trained practitioner will contact you to discuss your needs in more detail and agree on a treatment plan. This may be by phone or video.
- Begin treatment: Depending on your needs, you may be offered guided self-help, group therapy, or one-to-one CBT sessions. The IAPT programme is well-established, treating over one million people each year with strong evidence for recovery.
Pro Tip: Online self-referral is consistently the fastest way to get into the system. Avoid waiting for a GP referral unless your GP specifically recommends it, as self-referral is equally valid and typically quicker.
Choosing and booking private or online therapy
- Define your criteria: Use your priority list from the preparation stage to identify your non-negotiables.
- Search for accredited therapists: Look for therapists registered with BACP, UKCP, or NCPS. These are the main professional bodies in the UK, and registration means they meet regulated training and ethics standards.
- Review profiles and approaches: Most platforms and directories allow you to read therapist bios, see their specialisms, and understand which therapy approaches they use.
- Book an introductory session: Many therapists offer a shorter first session at a reduced cost. Use this to assess whether you feel comfortable and understood.
- Confirm confidentiality and data practices: Ask directly how your data is stored and whether your GP will be informed.
For a more detailed walkthrough, the guide to starting online therapy covers the full process from sign-up to your first session. If you want a broader view of the landscape, the guide to accessible online therapy is also useful. Additional self-help resources can support you between sessions while you are getting started.
What to expect and how to monitor your progress
After you have taken those steps to begin support, it helps to know what comes next and how to recognise real progress. Many people expect to feel better immediately, and when they do not, they assume the therapy is not working. In reality, progress in therapy is rarely linear.
What progress actually looks like
In the early stages of therapy, it is common to feel unsettled. Talking about difficult experiences brings them to the surface before they begin to resolve. Most people start noticing meaningful changes between sessions four and eight, particularly with CBT. Improvements tend to appear in this order:
- Cognitive clarity: You notice your thought patterns more clearly and can identify when you are catastrophising or avoiding.
- Behavioural changes: You begin taking small actions you previously avoided, such as going outside, making calls, or attending social events.
- Emotional regulation: Strong emotional reactions become shorter or less intense over time.
- Mood stability: Low or anxious periods become less frequent and easier to manage.
Tracking your progress using the PHQ-9 and GAD-7 questionnaires every two to four weeks gives you objective data to compare alongside how you feel day to day. Many online platforms include built-in mood tracking tools that do this automatically.
"Recovery is not a straight line. There will be weeks that feel like a step back. What matters is the overall direction of travel over several weeks and months."
The IAPT programme's evidence base shows strong recovery rates for those who complete a full course of CBT, with outcomes broadly comparable to medication for mild to moderate presentations. Completing the full course, rather than stopping early when you begin to feel better, is one of the most important factors in sustaining recovery.
When to consider switching or escalating
If you have attended six or more sessions and feel no change, it is reasonable to review your approach. You might consider exploring self-guided therapy tools to supplement your sessions, or reading about switching therapists if the therapeutic relationship does not feel right. It is also worth reviewing the types of online therapy available to you, as some people respond better to structured written therapy than to video sessions, or vice versa. Lack of progress is information, not failure.
Why most people give up and how you can break the cycle
Armed with practical steps and realistic expectations, it is worth addressing the real reasons so many people never follow through on mental health support. The most common explanation is not a lack of information. It is the absence of a clear next action and the weight of waiting.
Perfectionism is a significant obstacle. Many people spend weeks researching the ideal therapist, the best platform, or the right moment to begin, and then do nothing. Rigid thinking tells them that if they cannot do it properly, they should not do it at all. This is a trap. A slightly imperfect step taken today is worth more than a perfect plan that remains theoretical.
Long waiting periods also erode momentum. When someone self-refers to NHS Talking Therapies and then hears nothing for six weeks, it is easy to disengage. The key is to build in small, active steps during the wait. Using mental health management advice in the interim keeps you oriented toward recovery rather than passive waiting.
Every attempt builds self-trust. Even sessions that feel difficult or unremarkable are evidence that you are capable of seeking help. The act of trying, regardless of immediate outcome, is itself progress. Commit to one tiny next step today, book a session, complete a self-referral form, or read one therapist's profile. That is enough to start.
Take your next step to confidential support
If you are feeling ready to take that first small step, there is a direct and secure way to get started. Online therapy can often be accessed within 24 to 48 hours and is designed around your privacy and affordability needs.
MySafeTherapy connects you with UK-accredited therapists registered with BACP, UKCP, and NCPS. The sign-up process is straightforward, the pricing is transparent, and you can choose your therapist based on specialism, format, and availability. Sessions are available via video, chat, or avatar-based format to suit your comfort level, with evening and weekend slots available. If you decide to start therapy now, the platform guides you through every step. For a full overview of what is available, visit MySafeTherapy to explore your options with no obligation.
Frequently asked questions
How do I refer myself to NHS Talking Therapies?
You can refer yourself directly via the NHS Talking Therapies website without needing a GP appointment, or you can ask your GP to refer you. The self-referral process is straightforward and typically involves completing an online form describing your symptoms, with the service contacting you to arrange an assessment. The IAPT programme processes over one million referrals each year across England.
Is online therapy as effective as in-person therapy?
Evidence shows that online CBT is generally as effective as face-to-face delivery for mild to moderate anxiety and depression. The key factor is completing the full course of treatment rather than the format in which it is delivered.
What if I cannot afford private therapy?
NHS Talking Therapies are free for all UK residents and provide structured, evidence-based treatment. As research confirms, the NHS route is free but may involve a wait, while free self-help resources and peer support groups can provide meaningful support in the interim.
How do I know if therapy is working for me?
You should notice gradual improvements in mood, coping ability, and daily functioning over several weeks. Reviewing standardised measures such as the PHQ-9 every few sessions, alongside your own observations, provides clear evidence of whether therapy outcomes are improving for you.
