TL;DR:
- More than half of UK adults now prefer online therapy as their main mental health support.
- Virtual therapy, delivered via video or chat, is evidence-based and matches in-person outcomes for common issues.
- In-person care remains essential for severe mental health crises or complex trauma cases.
Over half of UK adults now consider online therapy as their primary route for mental health support, yet persistent myths about effectiveness and safety continue to hold people back. Virtual therapists are not a compromise on quality. They represent a structured, evidence-based model of care that has been adopted across NHS services and reviewed in clinical research worldwide. This guide sets out exactly what virtual therapists offer, how they compare with in-person sessions, where they perform best, and where their limits lie. Whether you are managing anxiety, depression, or recovering from trauma, the information here will help you make a clear, informed decision.
Table of Contents
- What are virtual therapists and how do they work?
- The key benefits of choosing a virtual therapist
- Are virtual therapists as effective as in-person therapy?
- When might a virtual therapist not be the right fit?
- Our perspective: Why virtual therapy is shaping the future of UK mental health
- Ready to try virtual therapy? Take the next step
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Flexible and accessible | Virtual therapists offer appointments outside typical working hours and eliminate the need for travel. |
| Evidence-based support | Online therapy platforms use proven approaches like CBT, EMDR, and ACT, often used in NHS programmes. |
| Consider limitations | Not all mental health issues are suited to virtual therapy, especially in crisis or for those with severe trauma. |
| Cost and convenience | Virtual sessions typically cost less than in-person therapy and offer more privacy. |
| Choose guided care | Outcomes are best with accredited, therapist-guided platforms, rather than self-guided or AI-only tools. |
What are virtual therapists and how do they work?
A virtual therapist is a qualified mental health professional who delivers therapy sessions remotely, using technology rather than a physical consulting room. The therapist holds the same accreditations and ethical obligations as any in-person practitioner. The primary difference is the medium through which sessions are delivered.
Most platforms use one or more of the following formats:
- Video calls via secure apps (similar to Zoom but built for clinical privacy)
- Text-based chat for asynchronous or real-time written communication
- Secure messaging apps with end-to-end encryption
- Avatar-based sessions for those who prefer anonymity
These formats are not simply a workaround for the absence of a clinic. They are purpose-built delivery channels for types of online therapy that include Cognitive Behavioural Therapy (CBT), Eye Movement Desensitisation and Reprocessing (EMDR), and Acceptance and Commitment Therapy (ACT). Therapist-guided platforms using video and secure apps deliver these evidence-based therapies effectively for UK adults across a range of presenting issues.
It is important to distinguish between therapist-guided and self-guided models. In a therapist-guided model, a registered professional leads each session, monitors progress, and adjusts the approach based on clinical judgement. In a self-guided model, the user works through structured digital content with limited or no direct therapist input. Research consistently shows that the guided model produces stronger outcomes.
The process of starting is straightforward. You complete an initial assessment, select a therapist based on your needs and preferences, and book your first session. Privacy is maintained throughout. Sessions take place wherever you have a stable internet connection, and confidentiality protocols match those required of any registered UK therapist.
The key benefits of choosing a virtual therapist
With a clear understanding of how virtual therapy works, we can examine why so many adults in the UK are choosing it, particularly given the demands of working and family life.
The practical advantages are significant and well-documented. Virtual therapy offers cost savings, with typical session fees between £50 and £80, alongside flexible scheduling including evenings and weekends, with no need to take time off work or commute. That last point matters more than it sounds. A 40-minute commute each way, combined with time in the waiting room, can turn a 50-minute therapy session into a three-hour commitment. Removing that barrier changes who can realistically access regular care.
| Benefit | Virtual therapy | In-person therapy |
|---|---|---|
| Evening and weekend access | Yes | Limited |
| No travel required | Yes | No |
| Session cost range | £50 to £80 | £60 to £120+ |
| Privacy at home | Yes | Clinic setting |
| Rural accessibility | Yes | Often limited |
For those living in rural or remote areas of the UK, where specialist mental health services may be hours away, flexible mental health support online removes a genuine structural barrier. The same applies to individuals with physical disabilities, caring responsibilities, or irregular work schedules.
Privacy is another factor that frequently influences the choice. Attending a therapy clinic involves being seen. For some people, that visibility alone is a barrier. Accessing support from home removes that concern entirely.

Pro Tip: Use self-help resources between live sessions to consolidate what you are working on with your therapist. Mood tracking and journalling tools can make each session more productive.
The virtual care benefits extend beyond convenience. Continuity of care improves when attendance is easier. You are less likely to cancel a session that requires no travel, no parking, and no rearranging of your entire afternoon.
Are virtual therapists as effective as in-person therapy?
Understanding the benefits, it is natural to ask whether virtual therapy can deliver results that genuinely compare with seeing a professional face to face.
The evidence on this point is now substantial. Guided online therapy can match in-person outcomes for common problems such as anxiety and depression, often requiring as little as three hours of direct therapist support when combined with structured self-help content. NHS IAPT services have integrated guided internet-based CBT and video-based interventions into standard pathways, which reflects the confidence that clinical bodies now place in these formats.
| Therapy format | Evidence base | Therapist contact | Best suited for |
|---|---|---|---|
| In-person therapy | Established | Full session | Complex or severe needs |
| Guided virtual therapy | Strong | Structured | Anxiety, depression, stress |
| Self-guided or AI models | Mixed | Minimal | Mild concerns, self-development |
"Online therapy delivered by registered professionals using evidence-based protocols produces clinical outcomes comparable to face-to-face care for the majority of adults with common mental health difficulties."
For anxiety, depression, and stress-related conditions, the comparison between in-person and virtual therapy is close. The therapy techniques used are identical. What changes is the environment in which they are applied.
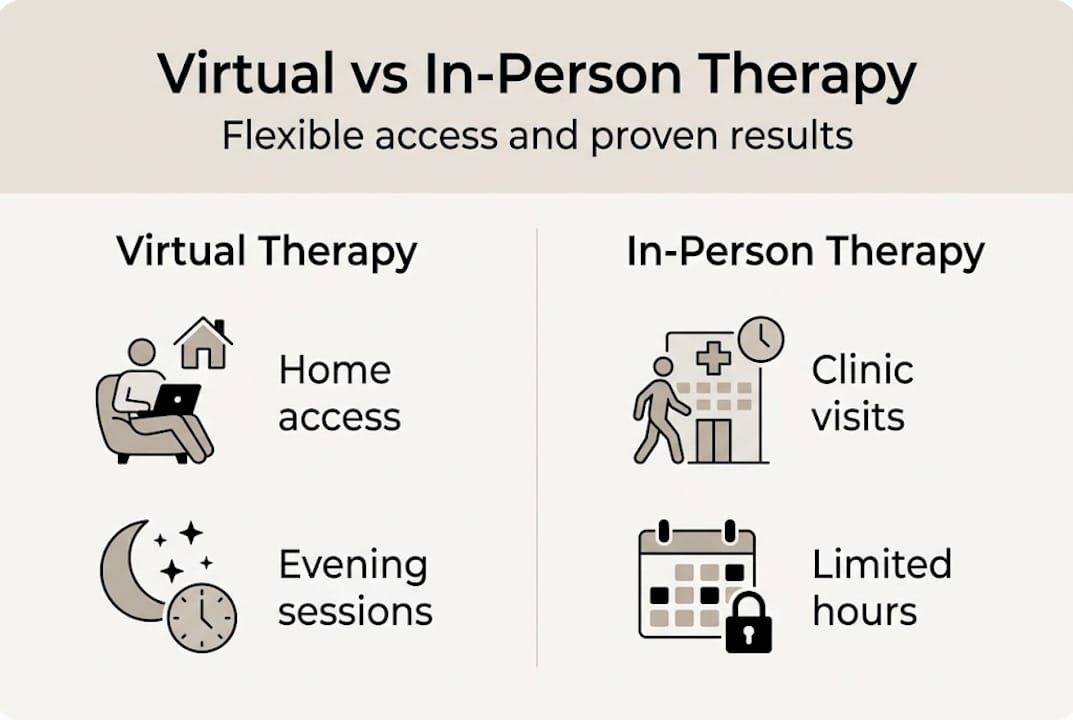
That said, self-guided therapy without professional involvement produces more variable results. Engagement tends to drop without the accountability of a scheduled session with a real person. Technology itself can also be a constraint. Poor connectivity disrupts sessions and affects the therapeutic relationship. Nonverbal cues are harder to read on screen, which can affect how quickly a therapist picks up on subtle shifts in a client's state.
Reviewing the NHS trials on iCBT makes clear that the platform structure and the quality of therapist involvement are the key variables. The technology is the delivery mechanism, not the therapy itself.
When might a virtual therapist not be the right fit?
While virtual therapy delivers well for many people, it is important to be clear about its boundaries and to recognise when another route may be necessary.
Certain situations call for in-person care. Virtual therapists may not be suitable for people experiencing severe or complex trauma, those in acute mental health crisis, or individuals who require somatic or body-based therapy where physical presence is central to the approach. Technology disruptions can interrupt care at critical moments, which is not acceptable in high-risk situations.
The following circumstances generally indicate that in-person or crisis support is more appropriate:
- Active suicidal ideation or self-harm requiring immediate intervention
- Severe psychosis or dissociative disorders requiring in-person clinical assessment
- Complex PTSD where body-based approaches such as somatic experiencing are clinically indicated
- Situations where home is not a safe or private environment for sessions
- Significant technology barriers, including unreliable internet access or lack of a private device
Practical limitations also apply. A reliable broadband connection, a private space, and a compatible device are minimum requirements. Without these, session quality is compromised and the clinical benefit is reduced.
The virtual care limitations are real and should be taken seriously. The fact that virtual therapy works well for many does not mean it is appropriate for everyone in all circumstances.
Pro Tip: If you are uncertain whether virtual therapy is right for your situation, speak with your GP first. You can also explore what to expect at each stage through a step-by-step guide to accessible online therapy before committing to a platform.
Our perspective: Why virtual therapy is shaping the future of UK mental health
The growth of virtual therapy is not a trend driven by convenience alone. It reflects a structural shift in how the UK understands and delivers mental health care. Waiting lists for NHS services remain long, and the gap between demand and capacity is not closing quickly. Virtual platforms, particularly those that are guided and evidence-based, offer a route to scale access in a way that traditional clinic models cannot.
The important distinction here is between guided and unguided formats. Evidence-based, guided platforms produce meaningful outcomes, while AI-only or purely self-directed tools show inconsistent results. The human relationship in therapy matters. Technology can support and extend that relationship. It cannot replace it.
The UK is in a unique position. NHS adoption of digital therapeutic pathways has given online therapy a clinical legitimacy here that is more advanced than in many other countries. That legitimacy matters. It signals to anyone still on the fence that virtual therapy is not a lesser alternative. For the right person, in the right circumstances, it is the most practical and effective route available. Exploring online therapy and AI tools together can also help you understand what supplementary support might look like alongside live sessions.
Ready to try virtual therapy? Take the next step
If you have read this far and recognise that virtual therapy could be the right fit, the next step is straightforward. MySafeTherapy connects you with UK-accredited therapists registered with BACP, UKCP, and NCPS, offering video, chat, and avatar-based sessions to suit your preference and schedule.
Sessions are available in the evenings and at weekends, with clear pricing and no long-term commitment required. Everything from your first assessment to your ongoing sessions is managed securely and confidentially. You can start therapy today or find out more about MySafeTherapy and how the platform works before making any decisions. The process is private, flexible, and built around your schedule.
Frequently asked questions
Is virtual therapy really as private as in-person therapy?
Yes. Reputable virtual therapists use secure, encrypted platforms and adhere to the same confidentiality standards required of all registered UK practitioners. Your sessions and personal data are protected throughout.
Can virtual therapy help with anxiety or depression?
For most adults, guided online therapy is effective for anxiety and depression, with clinical outcomes that closely match those achieved through face-to-face sessions with a registered therapist.
What if I need urgent or crisis support?
Virtual therapists are not equipped for emergency intervention. If you are in crisis, contact NHS 111, Samaritans on 116 123, or attend your nearest A&E. Virtual therapy is unsuitable for immediate crisis situations.
How do I choose the right virtual therapist?
Look for UK-accredited professionals registered with BACP, UKCP, or NCPS, and select a platform that offers evidence-based, guided therapy such as CBT or EMDR rather than unstructured or AI-only formats.
